“Decisions are part and parcel of a doctor’s life”
Deciding on interventions and treatments every minute: don’t like making decisions, then a doctor’s life probably isn’t for you, says
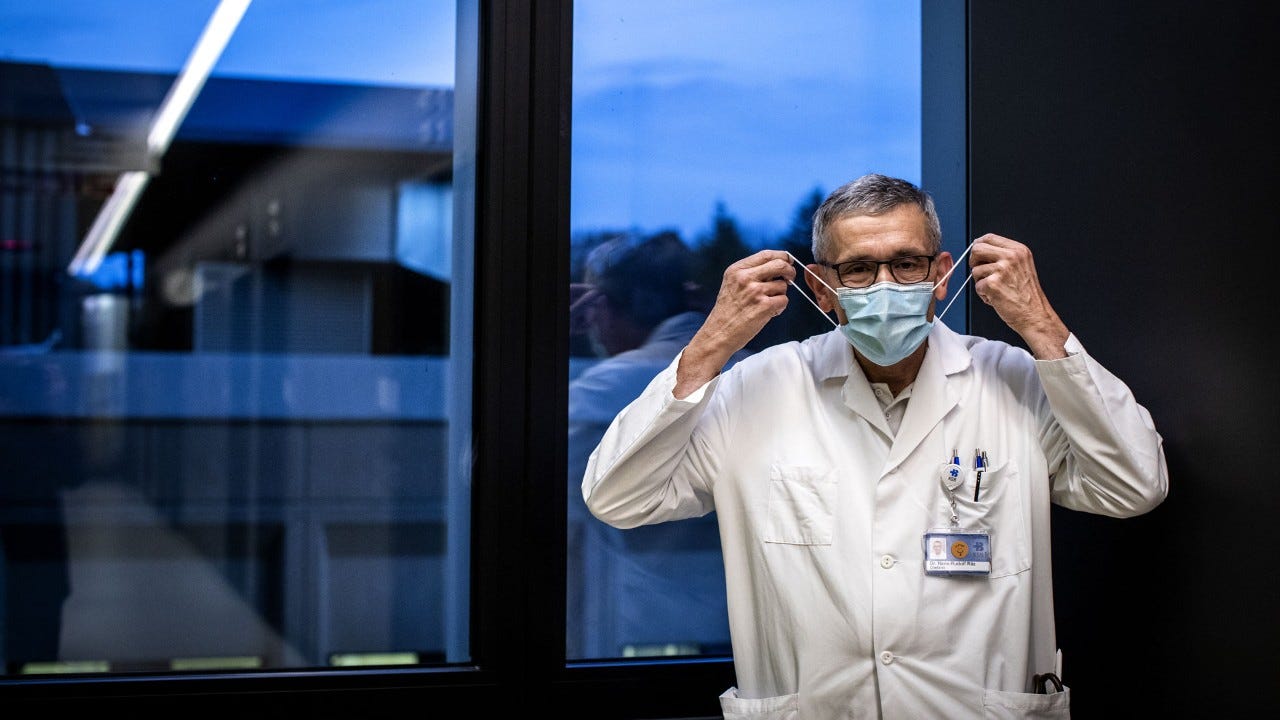
The dialysis centre at the Baden cantonal hospital is located in a big, bright room in a new development with huge windows overlooking neighbouring fields and trees. A beautiful sight that is good for the heart and soul. It’s late on Friday afternoon, and the hospital is relatively quiet after its usual hustle and bustle. Hans-Ruedi Räz is head of the department. He uses the quieter moments to visit his patients, and sits beside an elderly man. He asks how he’s doing, exchanges a few friendly words and wishes him a nice weekend. At that moment, another patient lets go of his cotton pad, which is supposed to stop the blood flow of a vein after dialysis. A gush of blood run down his arm and the bed he’s sitting on. Räz quickly pulls open a drawer containing bandages and goes to help the nurse who is looking after the elderly man who has had a bit of a fright. He soon calms down. Even small decisions sometimes have an important impact.
“As soon as you said hello, you had to have a plan in your head about how to proceed with the patient.”


Preventing the worst case
Making decisions, says Räz, is part and parcel of a doctor’s life: “If you don’t like making decisions, then a doctor’s life isn’t for you.” Räz saw this for himself as a medical student when he worked as a locum for family doctors at various medical practices. “In truth, as soon as you said hello, you had to have a plan in your head about how to proceed with the patient and make decisions incredibly quickly.” Stressful for a budding young doctor? “You learn, particularly with more experience, to consider all factors automatically. It’s all part of being a doctor. In fact, I can well remember that, even as a budding doctor, it was a good feeling for me to be able to make decisions myself,” laughs Räz.
Today, as a hospital nephrologist, he has a little more time for patient history and decision-making. But the decisions he makes are just as important as ever. For example, he is often faced with the question of whether to start kidney patients on dialysis at all or whether they should stop after many years of costly treatment. He also has to decide whether or not to register a patient for a kidney transplant. “These decisions,” says the 63-year-old, “are often risky and can lead to death.”
He was faced with a puzzling case just a few days ago. “The patient’s kidney failure was progressing very quickly. We didn’t know what the problem was. All the routine tests were negative, and nothing seemed to fit together,” says Räz. Then he did what he always does when faced with a difficult decision and is unsure about how to proceed: He put together an overview of all the medical facts available on the patient. He researched and read up. And he talked to colleagues. As he was putting together the information, a plan slowly formed in his mind and he was able to decide what to do: No immediate, potentially life-threatening drug therapy, but first stabilise the patient’s condition and do further tests. “Even if you don’t know everything at the moment, you have to consider what is reasonable given the current state of knowledge. And then I think: What’s the worst that could happen – and how can I prevent this from happening”, he says to describe the decision-making process. Top priority, even before the goal of helping the patient, is the goal of not harming them.
“High-risk cases are always discussed in inter-professional teams.”
Guiding ethical principles
Knowing how difficult and momentous medical decisions can be, Räz completed a master’s degree in ethical decision-making and trained as a moderator for case discussions. “High-risk cases,” he explains, “are always discussed in inter-professional teams along with the patient themselves and their relatives.”
In addition, Räz heads up the hospital’s internal ethics forum together with a speech therapist, where key existential questions are up for discussion. At present, the corona pandemic is forcing the expert committee to answer a seemingly unanswerable question: Who gets a space on the ICU ward when there are more patients than beds? Räz sighs. So far, thank God, they haven’t had to make this decision. If the worst came to the worst, they would stick rigidly to the ethical guidelines drawn up by the Swiss Academy of Medical Sciences (SAMW) which favours patients who have the prospect of more years of life ahead of them. In this case, an 80-year-old who is in great shape and still goes on mountain hikes does not necessarily lose out to a 50-year-old who not only suffers from COVID but also has a malignant tumour. The ethics forum, explains Räz, not only sets out the guidelines for decisions like these, but also offers practical assistance to individual colleagues by making inquiries with the patients’ family doctors or talking to their relatives, for example. “At the end of the day,” says Räz, “the doctor providing treatment is responsible for the case, but we are on hand to offer support if needed.”


Keep calm and carry on
We leave the dialysis ward in the new block and walk slowly through long carpeted corridors with black and yellow walls. The cantonal hospital’s A&E department and intensive care unit are still located in the old building. White is the dominant colour here, there is significantly less space and our shoes click on the linoleum floor. In an emergency on a busy day, decisions have to be made every minute: Is the patient who suffered a heart attack at risk of dying and needs to be moved to the crash room? Is the accident victim in a stable enough condition for surgery? Which ward should the young woman with serious injuries be moved to? In the intensive care unit, which now has 14 beds due to the corona crisis, there is a lot of activity – there’s no sign of anyone clocking off soon. All around there are groups of two, three or more people all discussing individual cases. Others are sitting in front of laptops studying endless information on patients that will form the basis of their decisions. The staff are also happy about every living will that is clear and comprehensible. Räz nods: "Above all, it is crucial for us to have a so-called medical representative who represents the patient's interests in precarious situations."
Although the ICU staff are under enormous pressure as a result of the corona crisis, the mood is surprisingly relaxed: friendly faces, frequent laughter; someone rubs their hands and arms with disinfectant, passes the bottle to a colleague and leaves the room with a spring in their step. Hans-Ruedi Räz calls this “professional composure”, which is essential in a hospital. What really makes their day is when a patient who was seriously ill returns to the hospital after their recovery to thank the staff for giving them a second chance at life: “Then we really know that we made the right decision.”
The job requires concentration, expertise and the energy to engage with each and every new case as they come in. Although Räz can now draw on many years of experience, it’s still a demanding undertaking. “But that’s all part of being a doctor. You can’t just decide not to make decisions,”