Balance disorders: causes, symptoms and treatment
We often take good balance for granted, but it’s a highly complex task. And our body sometimes makes mistakes, too.

Sometimes it feels like everything has turned upside down. It’s as if the world is spinning, the ground disappears from under your feet and you feel like you’re falling.
At times like this, your balance system has had a blip. Such malfunctions can occur for a variety of reasons – and are common. Almost one in four people will experience a balance disorder at least once in their life, with the risk increasing with age.
Dizzy spells like this can be worrying, which makes it all the more important to identify the symptoms and causes as quickly as possible and take the right action.
Vestibular system: what controls our sense of balance?
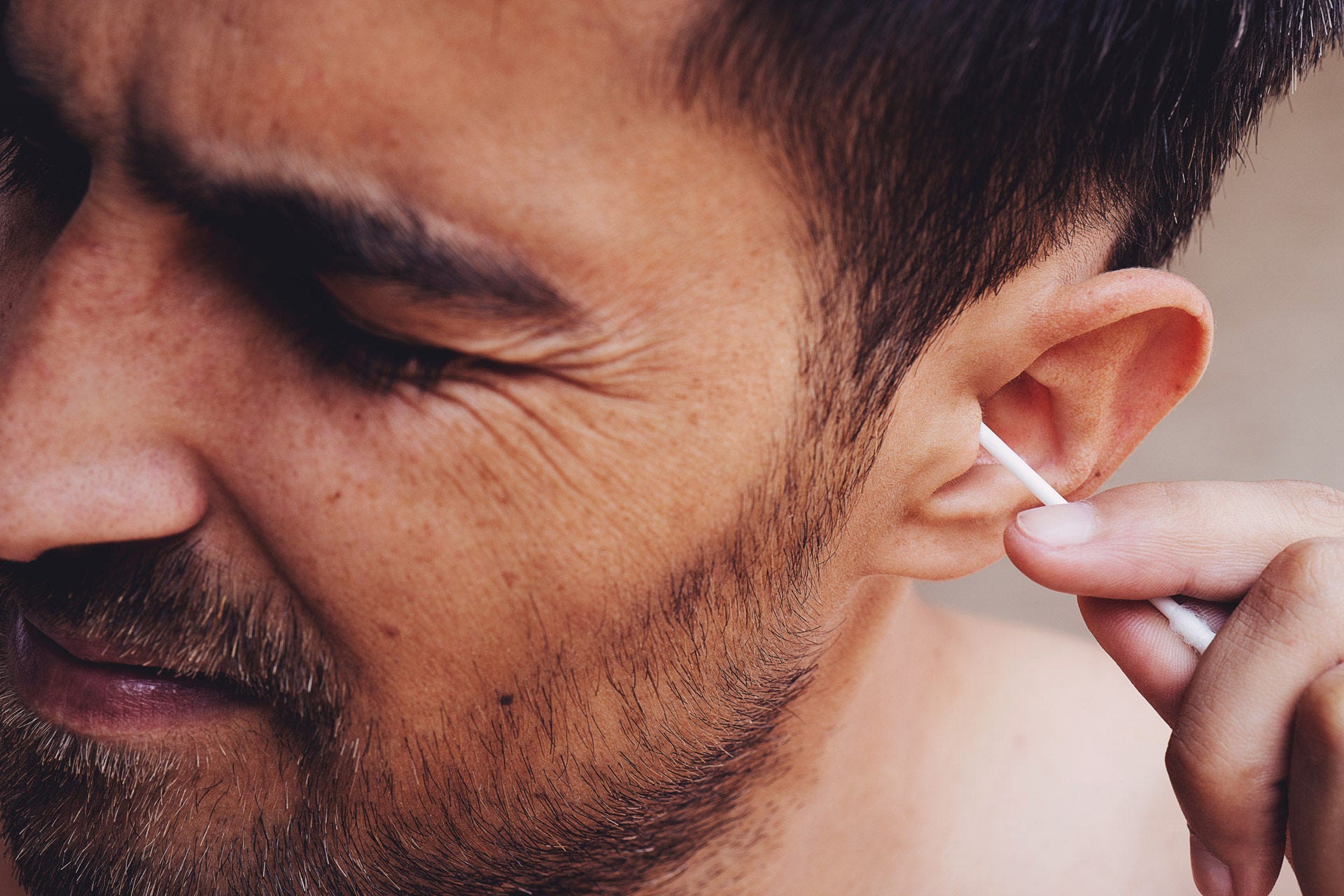
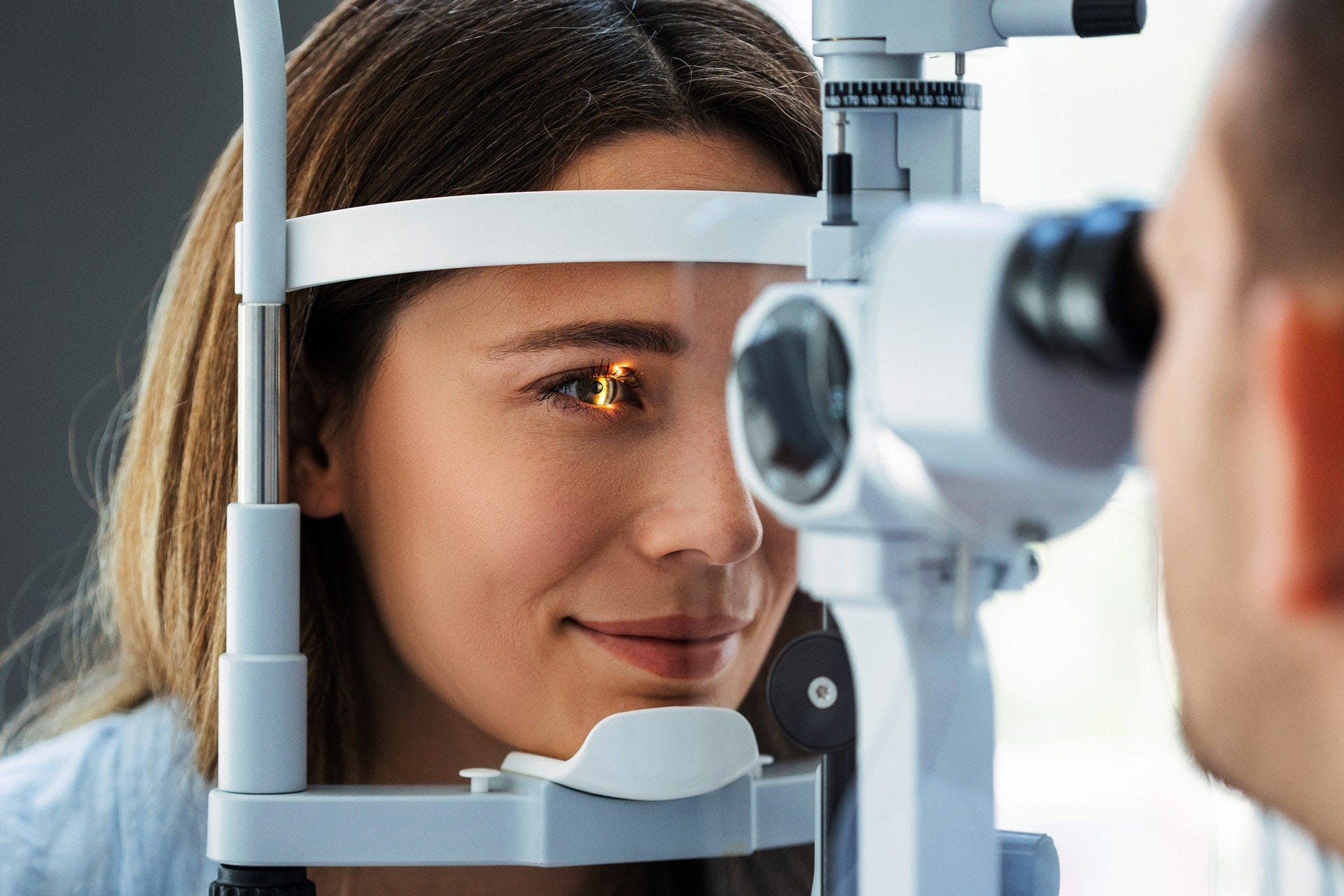
Three systems are responsible for our balance: the vestibular system, the eyes and proprioception.
The vestibular system is found in the inner ear. It consists, among other things, of three semicircular canals and hair cells which are connected to the vestibular nerve. The semicircular canals detect rotational acceleration in all three-dimensional planes.
The vestibular system sends information to our balance centre in the brain stem and cerebellum via the vestibular nerve.
“Dizziness is highly subjective.”
Additional information that is responsible for maintaining our balance is also gathered here: visual information provided by our eyes as well as the nature of the ground and the position of our joints, which are transmitted to our brain via proprioception.
Without proprioception, we wouldn’t be able to perceive how the movement, position or posture of our body relates to the earth and the space in which we find ourselves.
The balance centre in the brain stem and cerebellum then compares the information from the three sources and sends commands to the muscles of the eyes and musculoskeletal system to keep our field of vision constant and our body upright.
Dizziness as the main symptom
Dizziness can be triggered when our balance system receives contradictory information from the sensory sources.
Take reading in the car, for example. The vestibular system tells your brain that your body is moving, but your eyes report a static environment because you’re looking at the letters in the book. This contradictory information confuses the brain. It reacts with dizziness and nausea.
Dizziness – also known as vertigo – is an important symptom to show us that something isn’t right with the balance system . Julia Dlugaiczyk, ENT specialist, professor and joint head of the Interdisciplinary Centre for Vertigo at Zurich University Hospital, explains that dizziness is highly subjective.
“If headaches, double vision, facial paralysis or one-sided paralysis suddenly occur, special attention is required.”
Some people feel that the world is spinning around them, others feel more that their body is rotating, while others describe a swaying sensation like when you’re on a boat or going up and down in a lift.
Our perception of dizziness often becomes more diffuse with age, says Dlugaiczyk. “Many people affected then no longer perceive the dizziness as such, but often notice that they feel more unsteady when walking.”
Causes of balance disorders
There are many different reasons for disturbances in the balance system – often, several causes come together. This makes the work of Dr Dlugaiczyk and her team complex: “Once the patients have described their symptoms, the detective work to find the cause begins.”
Dlugaiczyk explains that the accompanying symptoms are often an indication of what is causing the disorder: If someone has hearing problems as well as dizziness, the cause is often in the inner ear, while the addition of headaches is often a sign that migraines are the trigger.
Alternatively, if the dizziness primarily occurs upon standing up, accompanied by a blackout, this suggests a cardiovascular problem as the cause.
“If headaches, double vision, facial paralysis or one-sided paralysis suddenly occur in addition to the dizziness, special attention is required,” says the doctor. In this case, the person could also be suffering from a stroke, which has to be treated quickly.
Disorders of the ear
However, a disturbance in the balance system is often primarily caused by an issue in the inner ear. These are the most common reasons for an ear disorder:
-
Benign positional vertigo
This can happen at any age, but the risk increases as we get older.
It happens when tiny ear stones (otoliths) detach from the vestibular system and enter the semicircular canals of the inner ear.
Typical movements that trigger positional vertigo include bending down to tie shoelaces or turning from one side to the other in bed.
These movements cause the otoliths to roll through the fluid of the semicirculer canal, which stimulates the hair cells in a way that doesn’t correspond to the body’s actual position.
This causes dizziness, which stops after 30 to 60 seconds when the otoliths stop moving. However, the dizziness is triggered again when you move again.
The good news is that specific repositioning manoeuvres can bring the otoliths back to their correct position in the vestibular system.
Patients can do these exercises themselves or with the support of a doctor or physiotherapist. Specialised treatment chairs are used for particularly stubborn cases. “The exercises help in over 90% of cases,” says Dlugaiczyk.
-
Middle ear infection
An infection in the middle ear can also affect the inner ear, where it can damage the hair cells in the hearing and vestibular systems. This can cause hearing loss and dizziness.
The vestibular nerves can also become inflamed – without the middle ear being infected.
Depending on the cause of the dizziness and the type of inner ear involvement, it is treated with antibiotics, anti-viral medication or steroids.
-
Benign changes in the vestibular nerve
“Benign changes can occur in the insulating layer of the vestibular nerve, the so-called myelin sheath, which can press on the auditory and vestibular nerves – and rarely also on the facial nerve,” says Dlugaiczyk.
The first symptom is usually deterioration of hearing in one ear and sometimes also problems with balance.
As long as these vestibular schwannoma don’t grow, they are checked regularly using magnetic resonance imaging. If they get bigger, surgery or radiation may be required.
-
Ménière’s disease
This disease typically involves spontaneous attacks of vertigo accompanied by hearing loss with ear pressure and a ringing in the affected ear (tinnitus). The attacks often last several hours.
While hearing and balance functions recover quickly after attacks in the early stages, the long-term course of the disease usually results in increasing hearing loss in the affected ear.
Despite extensive research, the actual cause of these recurring, extremely unpleasant attacks remains unclear. As is often the case in medicine, multiple factors are assumed to be involved.
Among others, genetic factors, autoimmune diseases and disorders of the fluid balance in the inner ear play a role. Overlaps with migraines are also observed.
One typical finding in patients is an excess of inner ear fluid – which can now be easily detected using magnetic resonance imaging. However, it is still unclear whether this is the cause, consequence or simply a side effect on the disease.
There is currently no stand-out treatment. Depending on the severity of the condition, step-by-step concepts are used to prevent vertigo attacks. These include pills or injections in the ear – if these don’t work, surgery on the ear may be required in rare cases.
Long-term consequences, such as hearing loss, chronic balance problems and psychosocial stress, are treated with a multi-modal therapy concept, such as hearing aids and counselling.
Disorders in other organs
It’s not only the vestibular system in the ear that can disrupt our balance. Various problems in our other organs can throw our sense of balance off kilter:
-
Cardiovascular diseases
The cardiovascular system supplies both the vestibular system in the inner ear and the balance system in the brain with oxygen and other nutrients. Cardiovascular diseases, such as high blood pressure or low blood pressure, can therefore also cause vertigo.
Cardiac arrhythmia and circulatory disorders of the brain, such as in the case of a stroke, can also present as dizziness.
-
Neurodegenerative diseases
When the neuronal functions in the brain deteriorate – as with dementia, Alzheimer’s or Parkinson’s, this can also affect the body’s system of balance.
-
Other neurological diseases
Other neurological diseases can also disrupt the balance system in the brain. Migraines are the most common, leading to dizzy spells as well as headaches. These are known as vestibular migraines.
Dizziness can also occur in the context of inflammatory diseases of the brain – for example, meningitis or multiple sclerosis.
-
Concussion
Trauma to the head, such as a concussion, can also cause dizziness.
There are several causes, including temporal bone fractures involving the bony labyrinth, a shock to the vestibular system or damage to the brain’s vestibular centre.
A blow to the head can also cause the otoliths to slip into the semicircular canals of the inner ear and trigger post-traumatic positional vertigo.
-
Psychological problems
Regardless of whether our world is “upside down” or the “ground is cut from under our feet”: The close and complex relationship between physical and mental balance is reflected not only in our everyday use of language, but also in many diseases of the balance system.
Dizziness can also be an important warning symptom of our body, which can subsequently trigger severe anxiety and accompanying symptoms such as a racing heart, sweating and fainting.
Conversely, anxiety and panic can also lead to dizziness, such as with panic attacks, fear of heights and agoraphobia (fear of wide, open spaces).
In the long term, such fears can lead us to avoid certain situations, such as gatherings of people or events with friends. This in turn can lead to social withdrawal.
Depending on the exact cause, psychological therapy methods are used. This is often cognitive behavioural therapy, less frequently also medication, as part of a multimodal therapy concept.
Balance disorders in old age
As we get older, our senses deteriorate as the performance of our cells and therefore also our sensory cells decreases. If the sensory input from our sensory cells deteriorates, contradictory information reaches the brain more frequently.
“As we get older, it becomes increasingly likely that we will experience balance disorders,” says Professor Julia Dlugaiczyk. There are many reasons for this: In the inner ear, the number of hair cells and nerve fibres of the vestibular nerve decreases.
In addition, the otoliths become brittle so that they can detach from their lower surface more frequently and cause positional vertigo.
And the balance centre in the brain stem and cerebellum is more frequently affected by neurodegenerative diseases or circulatory disorders in old age. As a result, our brain processes balance stimuli more slowly. This means that our body balance is no longer able to adapt as quickly to changes in the environment, so the risk of falling increases.
However, the loss of function in old age not only affects our sense of balance, but also other important sources of information, such as our vision, proprioception and spatial orientation through hearing. “Together with the decline in muscle mass and the increasing problems of the musculoskeletal system, this leads to complex balance problems often referred to as senile dizziness,” says Dlugaiczyk
.
But Dlugaiczyk says that the term “senile dizziness” is misleading, “because it gives the impression that it’s part and parcel of old age, and you just have to accept it. Fortunately, this isn’t true in many cases.”
With an interdisciplinary specialist assessment and the appropriate therapies, those affected can reduce their risk of dizziness and the associated risk of falling. Sometimes it is actually “only” undetected positional vertigo, which can be treated quickly and effectively, says Dlugaiczyk.
Medication also often leads to balance disorders and associated gait problems. Certain medicines increase the risk of falls among older people. Dlugaiczyk recommends having side effects and interactions of the medication checked at the family doctor’s practice and consulting a specialist if there are any problems.
Other causes
External influences can also disturb our balance. These include:
-
Alcohol
Alcohol impairs balance control on several levels.
Firstly, it has an acute and direct effect on our vestibular system. Here, it leads to incorrect stimulation of the semicircular canals, causing dizziness, particularly when lying down.Alcohol also has an acute effect on the cerebellum. This part of the brain controls our coordination and the movement of our body and eyes. If the cerebellum can no longer function properly, the well-known symptoms occur: unsteadiness, an unsteady gait, and coordination problems.
Alcohol also damages the nerve fibres that are primarily responsible for proprioception – how we perceive the position, movement and orientation of our body in space.
People who chronically consume too much alcohol permanently damage their cerebellum. Such overconsumption also leads to restrictions in the proprioception of our feet and legs, which increases gait instability.
-
Medication
Various medications have side effects that can trigger feelings of dizziness.
For example, some drugs, such as some antibiotics or diuretics, damage the sensory cells in the vestibular system
,
while other substances suppress the activity of the balance system in the brain. These include tranquillizers, sleeping pills, muscle relaxants, anti-epileptics, migraine medication and antidepressants.
Excessive doses of antihypertensives can also lead to dizziness.
-
Travel sickness
Travelling can also upset the vestibular system in the inner ear, be it the swaying ground on a ship, a curvy mountain pass in the car or turbulence in a plane.
In such situations, the sensory channels sometimes send contradictory information to the brain. When the brain can’t make sense of the information it receives, it is known as a sensory mismatch.
Training balance: exercises
No matter your age, our senses like to be trained! If we don’t use them, they deteriorate. The same applies to our sense of balance:
-
Exercising outdoors
“An active lifestyle with plenty of exercise outdoors is the best way to train your sense of balance,” says professor Julia Dlugaiczyk.
Even taking regular walks in the wood can help. The changing ground underfoot is great for training balance. Forest floors can be uneven, steep, hard and soft, which is great for our sensory proprioception – the input that our feet and joints in particular send to the brain.
This information is important so that the balance centre in our brain can form a picture of how our body is positioned in relation to the earth and where we are.
For anyone looking for a little more action, Dlugaiczyk recommends one of the many vitaparcours trails in Switzerland.
-
Music and dance
Go dancing more often! When we dance, our brain has to coordinate many different processes in the body, so our brain activity is correspondingly high and complex. Among other things, this boosts our cognitive capacity – and our balance.
-
Play with balls
The simplest exercise is to throw a small ball against a wall. Change the surface you stand on: play on the ground, then on a mat.
Or you can play a different ball game. “Ball sports are great for training our postural control, stabilising our field of vision and improving hand-eye coordination,” says Dlugaiczyk.
-
Practice balancing
There are also many exercises for training balance at home. Stand in the corner of a room without touching the walls. This is for safety in case you lose your balance.
Step 1: Roll on to your toes and stay here with your heels lifted.
Step 2: Stand on one leg and pull the other knee towards your chest. Hold for a few breaths. Then switch sides.
Step 3: Walk in a straight line, placing one foot in front of the other. You can increase the difficulty by changing the surface and adding obstacles.
-
Specialised balance physiotherapy
“Specialised physiotherapy is the most effective therapy we have available for many forms of balance disorders – and the best way of preventing falls,” says the expert Dlugaiczyk.
In technical jargon, this is often referred to as “vestibular physiotherapy”. Depending on the diagnosis and severity of the balance disorder, specially trained therapists take patients through individual training programmes tailored to the requirements of their daily routine.
Close cooperation between patients, physiotherapists and doctors is essential here to be able to react quickly to any changes and adjust the training programme accordingly.
Further tips for prevention
There are numerous ways to avoid dizziness and prevent balance disorders – and to promote the function of your sensory organs:
- Drink enough water. At least two litres a day.
- Get enough sleep on a regular basis.
- Eat a balanced diet with plenty of fresh ingredients.
- Drink less alcohol. It is proven that even the smallest quantities of alcohol are harmful for health.
- Take time out Yoga, meditation or other methods of mindfulness help us to regain our inner and outer balance.
- Exercise regularly – whatever your age. The World Health Organisation (WHO) recommends that adults aged 18 to 64 years do at least 150 to 300 minutes of moderate-intensity physical activity per week. Alternatively, 75 to 150 minutes of vigorous-intensity exercise per week is sufficient.
- If possible, avoid medication that affects your balance, especially sleeping pills or sedatives.
Video: 5 simple balance exercises
Diagnosis and treatment
There are numerous causes of balance disorders, and the diagnosis can vary accordingly. “The first point of contact is your family doctor practice,” says Dlugaiczyk. “In most cases, the medical history provides a clear indication of the cause.” Based on the information gathered, the family doctor then refers the patient to a specialist.
If there is a problem with the inner ear, they will be referred to an ear, nose and throat specialist (ENT). If the cause is a neurological disorder, a neurologist can help. If a visual impairment leads to balance problems, an ophthalmologist will provide treatment. And cardiovascular-related causes are treated by an internist or maybe a cardiologist.
There are also interdisciplinary facilities such as the Interdisciplinary Centre for Vertigo and Neurological Visual Disorders at Zurich University Hospital. Specialists from several disciplines work together there: Ear, nose and throat medicine, neurology, ophthalmology, psychiatry and psychomatic medicine as well as physiotherapy.
If necessary, the centre also brings in colleagues from other disciplines. "In this way, we ensure that our patients suffering from vertigo receive tailored diagnostics and treatment to get them back on their feet.
Even if not every case of vertigo can be cured, in most cases the quality of life can be significantly improved,” says Dlugaiczyk. The centre is open to patients with all types of dizziness – from “simple” positional vertigo to complex balance disorders.