Psoriasis: causes, symptoms, treatment
Some 170,000 people in Switzerland suffer from psoriasis, making it one of the most common skin complaints. How can the symptoms be eased?
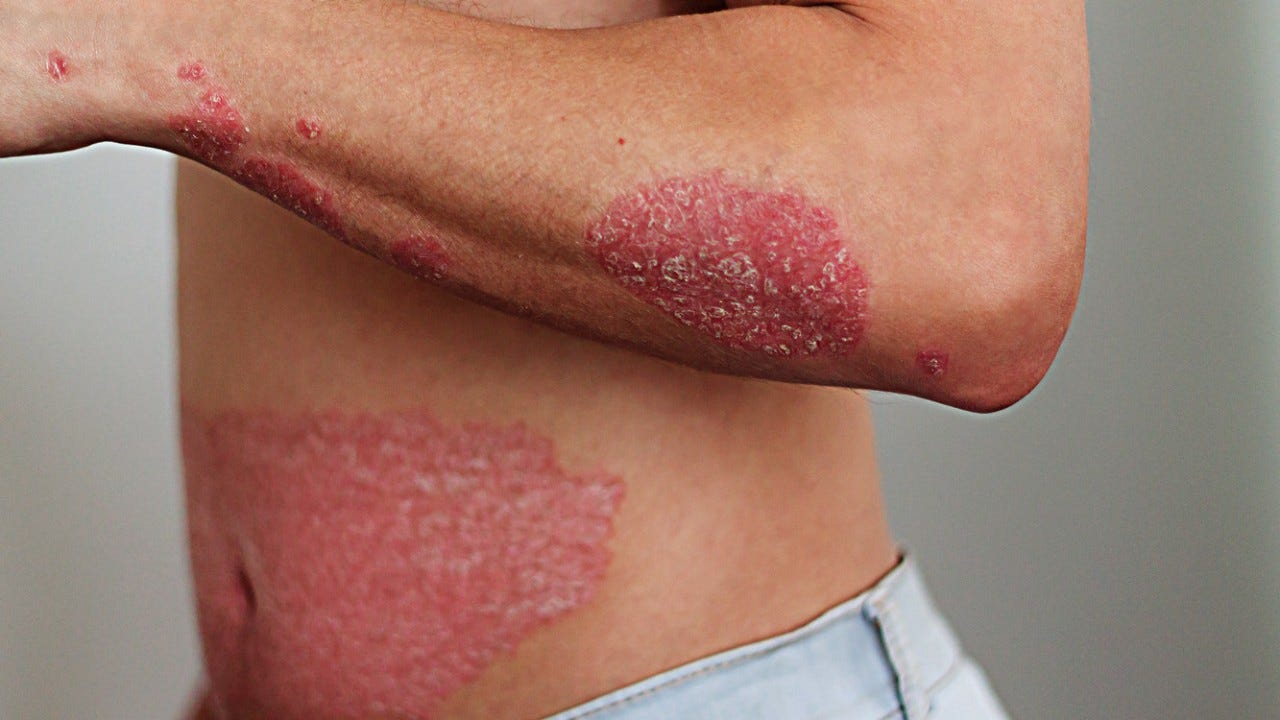
Psoriasis is a chronic inflammatory skin disease that is not contagious. Psoriasis vulgaris (also known as chronic stationary psoriasis) is the most common form, with red and scaly patches of skin that have a silvery sheen and may be itchy. The spread of these scaly patches varies from person to person.
While some people only have patches on a few areas of their body, for example on their elbows, knees or scalp, others may suffer from a serious condition which can affect the whole body. These patches occur when skin cells grow too quickly. With healthy skin, this process takes 28 days but the cells in psoriasis patches are regenerated in just 8 days. The affected areas dry out and tear, which can be painful. Why does the skin react in this way?
“Psoriasis is an autoimmune disease. This means that the patient's own immune system activates itself due to misdirected signals without the help of external pathogens," explains Prof. Wolf-Henning Boehncke, chief consultant of dermatology at Geneva University Hospital. Psoriasis is neither contagious nor an indication of a lack of hygiene. It is simply an inflammation of the skin.”
As psoriasis mainly affects the skin and is thus a visible disease, patients often also suffer high levels of psychological distress. “People suffering from psoriasis are subject to many prejudices. One of my patients was even ordered out of an outdoor pool by a lifeguard. This is totally unacceptable. The public needs to be better informed." In guides from the Swiss Psoriasis and Vitiligo Society (SPVG), for example, sufferers can find helpful input on how to deal with their disease.
“Psoriasis is neither contagious nor an indication of a lack of hygiene.”
Causes of psoriasis
It is not known what triggers psoriasis. What we do know is that this inflammatory disease isn’t inherited, only the predisposition to it, which means there is no psoriasis gene. “In fact, the genetic influence is rather small,” says Professor Boehncke. And an inherited predisposition doesn’t necessarily lead to the onset of the disease. Various genes and additional triggers are involved. The following causes, among others, play an important role:
- Psychological stress (with 40 to 60% of those affected not responding to stress)
- Infections and diseases (particularly glandular fever, streptococcal angina or skin germs)
- Mechanical skin irritations, such as friction, pressure points and injuries.
- Metabolic disorders
- Hormonal factors
- Smoking
- Excessive alcohol consumption
- Medication (e.g. malaria medication, beta blockers, lithium)
- Obesity
- Environmental factors
Symptoms and concomitant diseases
The course of psoriasis varies considerably from person to person and occurs in phases. There are always times in which it is better or the scaly patches disappear completely. “Even without treatment,” says Boehncke. “But the improvements are never permanent.”
A phase usually starts with small, inconspicuous changes to the skin. The papules (nodular thickenings of the skin) begin to flake and spread to plate-sized patches. In the most severe cases, the person’s entire skin may turn red, but this is very rare. Psoriasis also often occurs on the scalp, fingernails and toe nails.
And concomitant diseases, known as comorbidities, are also possible. These may or may not be related to psoriasis:
-
Psoriatic arthritis
“Around a third of patients develop psoriasis arthritis,” says Professor Boehncke. This is painful inflammation of the joints, spine, bursae, tendon insertions or tendon sheaths.
Typical symptoms include stiffness in the morning, pain while at rest and swelling. “In the vast majority of cases, psoriasis affects the skin first before the joints. That’s why it’s important to quickly see a dermatologist so the symptoms can be managed in good time.”
-
Cardiovascular diseases
It puts you at greater risk of cardiovascular diseases, particularly high blood pressure and heart attacks.
-
Obesity
There is interplay here, with obesity being a major risk factor for psoriasis on the one hand, but also a concomitant disease on the other. Obesity also increases the risk of high blood pressure, diabetes and cardiovascular diseases.
-
Diabetes mellitus type II
Diabetes is a chronic disorder of the blood sugar metabolism. As there is constantly too much sugar in the blood, vessels and organs are damaged. Psoriasis patients are at a higher risk of diabetes.
-
Metabolic syndrome
Metabolic syndrome is the medical term used when a person suffers a combination of three metabolic disorders, such as obesity, diabetes, high blood pressure, and disturbed fat or sugar metabolism.
-
Chronic bowel diseases
Although inflammatory bowel diseases such as Crohn’s disease are rare, they are nevertheless more common in psoriasis patients than non-affected individuals. A typical symptom of Crohn’s disease is recurrent diarrhoea, sometimes with cramp-like pains.
-
Depression
Mental illnesses, especially depression, are also common among those suffering from psoriasis. “However, these aren’t depressive moods due to appearance, but endogenous or “classic” cases of depression,” says Boehncke.
Treatment of psoriasis
Although psoriasis can’t be cured, it is very treatable. Professor Boehncke explains: “With the treatments available today, the visible patches disappear entirely for most patients. Or they reduce to the extent that only trained eyes can recognise them.”
-
Topical therapy
Milder forms of psoriasis are treated locally with creams and ointments.
-
Phototherapy
For moderately severe symptoms, phototherapy may be an option. With this treatment, the skin is exposed to UVA and/or UVB light over a period of several weeks, sometimes in combination with medication or baths.
-
Systemic therapy
Medication is usually only prescribed in severe cases, because although the drugs are effective, in rare cases they can have very serious side effects.
-
Biopharmaceuticals
Biopharmaceuticals are a newer form of treatment. They are administered into the bloodstream in the form of injections or infusions and act directly on the immune system. “Biopharmaceuticals have revolutionised treatment options.
They are much safer and more effective then conventional therapies, because they very specifically block certain inflammatory messengers,” says Wolf-Henning Boehncke. The biopharmaceuticals neutralise the messenger substances, thus stopping the inflammation.
-
Climatotherapy
One non-medicinal remedy for psoriasis is climatotherapy, i.e. a longer stay in the mountains or at the sea, especially the Dead Sea.
“Twenty years ago, the treatment options were limited, but today there are only very few patients who can’t be treated.”
Home remedies for psoriasis
It can be a good idea to try home remedies for minor ailments such as a cough or sore throat, but Professor Boehncke strongly advises against this for psoriasis. “Psoriasis not only affects a person’s skin and mental health, but also the cardiovascular system.”
So it’s important to treat psoriasis properly. “Twenty years ago, the treatment options were limited, but today there are only very few patients who can’t be treated. Psoriasis patients who haven’t seen their dermatologist in a while would be advised to go back.”
Complementary medicine also offers various therapeutic approaches, for example hydrotherapy or traditional Chinese medicine (TCM). But it is by no means a substitute for seeing a specialist. Anyone suffering from psoriasis should avoid spicy food, excessive alcohol consumption and smoking.
A balanced diet is recommended, with plenty of fruit, vegetables and omega-3 fatty acids such as fish and rapeseed oil. And finally, relaxation and reduction of stress are good for the soul and can have an impact on the course of the disease. How a person chooses to relax and unwind varies as much as the disease itself and the therapy used to treat it.


